A sessional instructor and business professor study the reinvigoration of a Toronto hospital and discover the secret(s) of its success from a public management perspective. They determine what this facility, which now specializes in rehabilitation and complex care cases, was doing right from the very start.
It’s not every day that a hospital, on the brink of termination, is reborn. It’s a complex endeavour. You need a water-tight value proposition, proving there’s a void to be filled, as well as healthy finances and stakeholder buy in. Pinpointing the most effective systems and partnerships in this mammoth undertaking would be helpful – priceless, in fact – as this information could inform similar operations by providing a template for success in public management and infrastructure governance.
Enter Sessional Instructor Sherena Hussain and Professor James McKellar of the Schulich School of Business. They carried out just such a venture; they conducted a case study of Bridgepoint Active Healthcare, a 464-bed rehabilitation and complex care hospital affiliated with the University of Toronto, which re-opened its doors in April 2013. Now part of the Sinai Health System, Bridgepoint is the single largest organization in Canada to focus exclusively on research, care and teaching for people with complex health conditions.

In wondering what made this reimagined hospital such a triumph, the researchers focused on the use of public-private partnerships (PPP) for social infrastructure. They discovered success with PPPs was about people; Hussain and McKellar’s research uncovered the role of personalities, relationships and strong leadership in bringing a successful project to fruition in the face of complex, intersecting challenges.
“The PPP is only one variable in explaining the overall success of this complex and highly visible social infrastructure project,” Hussain explains.
The findings of this research were published in Public Works Management & Policy (2020).

Bridgepoint almost closed in 1997
Healthcare is a high-stakes sector. There have been, historically, tensions between hospitals, seeking to retain independence, and the province. Ontario exclusively funds the delivery of healthcare services including hospitals, although doctors remain as private entities. Hospitals are run by independent boards of directors that oversee the quality of patient care and undertake complex building programs, etc. (Canadian Medical Association).
The case of Bridgepoint was a nail-biter: In 1997, the Ontario government planned to close the existing hospital and transfer its patients to other long-term care facilities. Marian Walsh, Bridgepoint’s then president and CEO, faced a formidable challenge: How to save Bridgepoint. She did it and, as Hussain and McKellar prove, how she did it is well worth studying.
How did the researchers approach their work?
Hussain and McKellar first conducted a literature and archival review of key policy submissions, project documents, private sector agreements and financial disclosures spanning back to late 1990s.
Following this, the two conducted over 40 semi-structured interviews, from 2013 to 2019, with government officials, hospital board members and senior management, private contractors, advisors, politicians and stakeholders involved in Bridgepoint.
Four ingredients to the success of Bridgepoint
Through this rigorous analysis, Hussain and McKellar determined that there were four ingredients that contributed to the success of Bridgepoint’s rebirth, under Walsh’s oversight, which involved the ambitious construction of a new facility.
Ingredient 1: A social license to operate
A social license refers to ongoing acceptance of an institution or company’s business practices and procedures by its employees, stakeholders and the general public. It exists when a project has overarching approval within the local community and broad social acceptance. This was something that Walsh recognized and emphasized.
“The result is that community members become advocates of the project as they consider themselves to be co-owners and emotionally vested in the future of the project; such is the strength of self-identification,” said a member of Bridgepoint staff in a 2016 interview.
Ingredient 2: Strong leadership
Walsh provided strong leadership that “embodied in clarity of purpose, tenacity, interpersonal skills, effective communication skills, management of governing bodies, and a vision,” McKellar emphasizes.
Walsh was respected by many stakeholders and became “the glue among the project components that transcended legal agreements,” according to a Mount Sinai senior executive interviewed in 2015.
Ingredient 3: A clear vision
The vision for success was driven by two fundamental pledges, say Hussain and McKellar: a commitment to a hospital environment that directly addressed the special needs of various stakeholders, and a commitment to a surrounding community in need of economic and social renewal.

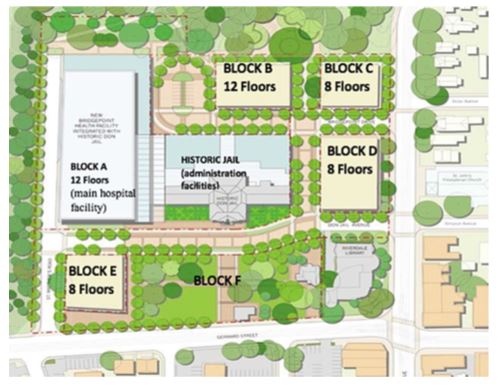
Ingredient 4: An architectural statement that embodies the vision
This new facility, featured in many architectural publications, served an important symbolic as well as functional role, extending beyond the physical buildings.
In realizing the merits of Bridgepoint and analyzing its success, the researchers provide tips for future ventures in public management – be they in the healthcare or other sectors. “The facility was instrumental in stimulating community-level revival and health care transformation, while also assisting in Bridgepoint’s strategic positioning and serving as a template for future social infrastructure,” Hussain states.
To read the article, visit the website. To learn more about Hussain, visit her profile page. For more on and McKellar, visit his Faculty profile page.
To learn more about Research & Innovation at York, follow us at @YUResearch; watch our new animated video, which profiles current research strengths and areas of opportunity, such as Artificial Intelligence and Indigenous futurities; and see the snapshot infographic, a glimpse of the year’s successes.
By Megan Mueller, senior manager, Research Communications, Office of the Vice-President Research & Innovation, York University, muellerm@yorku.ca